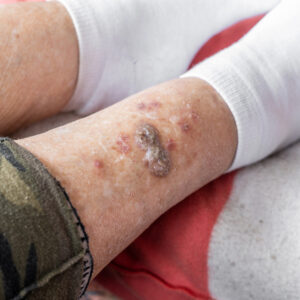
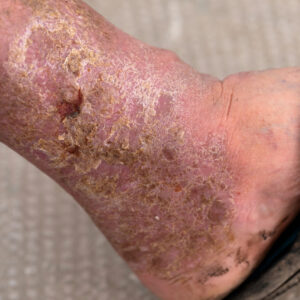
Understanding Pressure Ulcers: Prevention and Treatment Introduction Pressure ulcers, also...
Read More
Wound Care Center
A Specialized Facility for Wounds That Refuse to Heal
Not all wounds abide by the rules. They hang around weeks, do not respond to conventional dressings, and silently deteriorate as patients go around urgent care visits and primary care visits without receiving actual answers. Our Wound Care Center is designed to cater to those patients at Heart and Health Medical.
Our center is based in Massapequa, covers communities across Long Island, and has a board-certified surgeon and a fellowship-trained podiatric specialist with clinical experience spanning more than 30 years. We treat the wound in front of us and investigate the systemic conditions behind it.
When the wound on your body has not improved in any way in 14 days, that is your alarm. The possibility of deep infection, bone involvement, and possible loss of limb increases significantly within 30 days of non-progressive improvement.
Wound Care Center
If you have a wound that has not started to heal within 14-days. Schedule a consultation with a wound care specialist immediately.
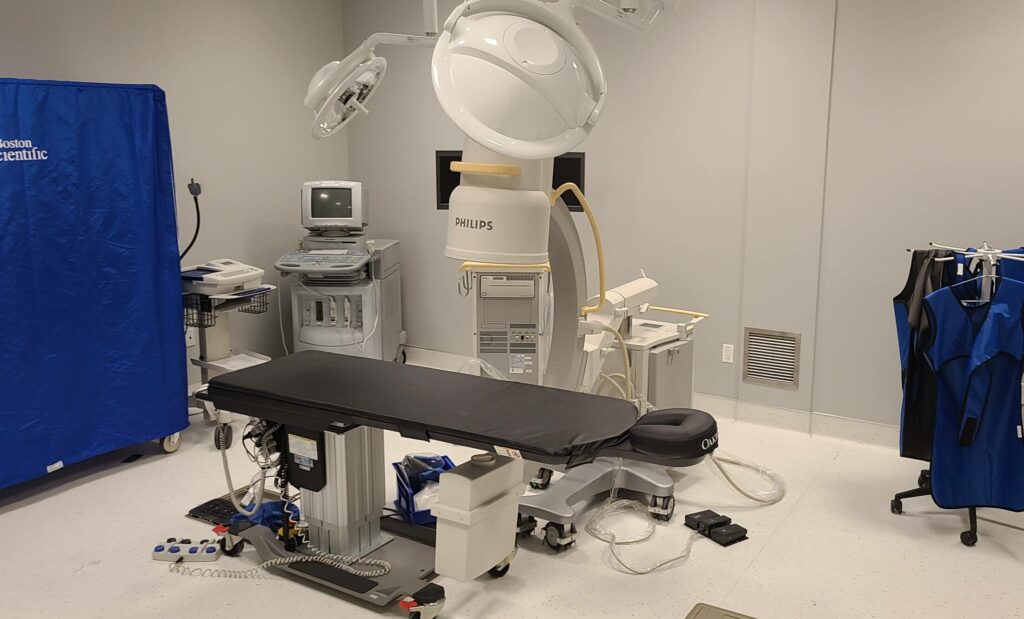

What Makes a Wound Chronic
A chronic wound develops when the process of healing the wound does not go through its stages. In normal conditions, the process of healing passes through four overlapping stages that include an initial clotting stage, an inflammatory stage whereby the tissue is cleared of debris and bacteria, a proliferative stage where the new tissue is produced, and a remodeling stage whereby the new tissue matures and strengthens.
The one stage relies on the previous stage.
These phases stall or malfunction when the patient is diabetic, has circulation difficulties, nerve damage, or nutritional deficiencies. The inflammatory phase can become too prolonged, such that the proliferative phase never gets a chance to take off.
Instead of forming new collagen, the tissue that is supposed to be doing so is breaking down further. The wound bed is filled with slough and dead tissue and occasionally a biofilm-protective coating, which bacteria deposit around themselves in order to protect themselves against antibiotics and the immune response.
These underlying disruptions cannot be dealt with by the use of normal wound dressings.
Cure is not a mere case of keeping the wound clean and covered. It involves determining and rectifying the biological environment that is not allowing closure.
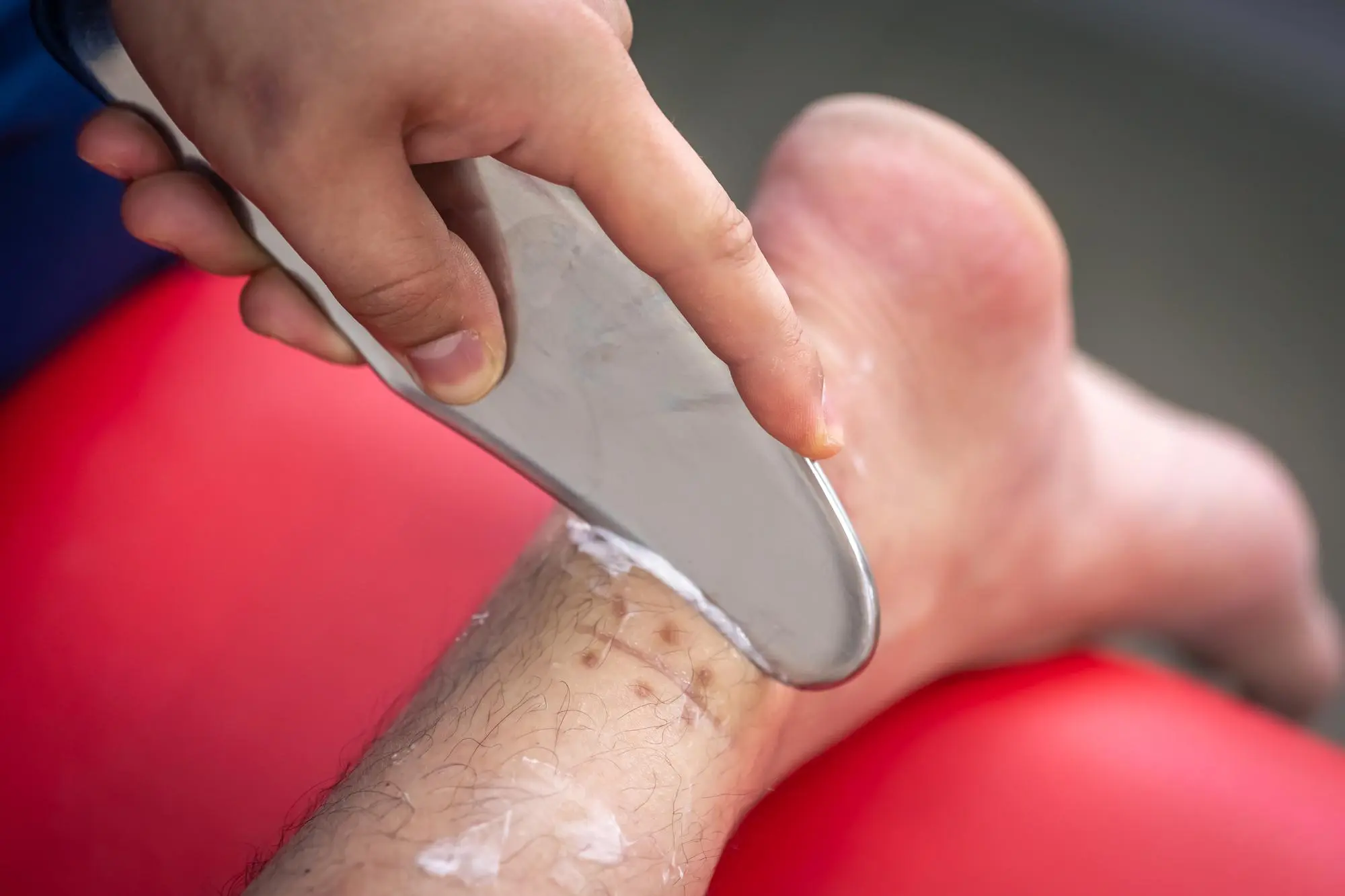
Wound Types Treated at Heart and Health Medical
Diabetic Foot Ulcers
The most common chronic wound in clinical practice is diabetic foot ulcers.
Increased blood glucose destroys small blood vessels in the body, decreasing blood oxygen delivery to the peripheral tissues. Meanwhile, diabetic neuropathy removes the pain message that would otherwise communicate an injury to a patient.
The outcome is the development of wounds to the sole, heel, or between the toes without the patient experiencing the development.
When a diabetic foot ulcer is discovered, it may be deep enough to reach subcutaneous tissue or tendon.
These wounds develop osteomyelitis – infection of bone without aggressive therapy, which puts the threat of amputation dramatically high. We use a mix of wound debridement, offloading, infection control, vascular inspection, and liaising with the endocrinologist of the patient to balance glucose and the wound.
Venous Leg Ulcers
Venous leg ulcers occur when the valves in the lower leg veins cease to work effectively. Blood that would be pumped upwards to the heart accumulates in the leg and results in continued pressure on the small vessels beneath the skin. With time, such pressure causes fluid and proteins to move into the surrounding tissue, leading to chronic inflammation and skin breakdown, leading to an ulcer.
The wounds are normally found on the inner lower leg, above the ankle and are usually irregular and shallow with a weeping appearance. The skin around the area tends to exhibit chronic venous disease, brown discolouration, thickening, and hard or woody surface known as lipodermatosclerosis. When the wound surface is treated without correcting the venous insufficiency that is causing it, it will recur. Both are assessed by our team.
Arterial and Ischemic Ulcers
Arterial ulcers are caused by the presence of insufficient blood flow, whereas venous ulcers are caused by excessive pressure. Peripheral artery disease causes constriction of the arteries that serve the legs and feet, due to the formation of atherosclerotic plaque. Ulceration starts when the delivery of oxygen to tissues is below the level required to maintain cell viability.
Arterial trauma is usually seen on the toes, heels and the bony prominences of the foot. They are usually hard, pale and painful – especially during rest or when the leg is raised. The surrounding skin can be cool and devoid of hair. Without proper perfusion, these wounds will not heal, and this is the reason as to why a vascular assessment is a non-negotiable initial step in our assessment plan.
Post-Surgical Wounds
The surgery that opens, opens or becomes infected after the operation necessitates some form of attention than the normal post-operative care.
Causes of wound dehiscence may include failure of the suture, infection, hematoma or factors in the patient such as steroid use, malnutrition or uncontrolled diabetes.
These injuries require an adequate debridement, infection control, and in many cases advanced methods of closure. We coordinate care with the surgeon of the patient to help in moving these wounds towards closure and do so in an efficient manner.
Radiation Wounds
Radiation therapy damages not only the cancer cells it targets but the blood vessels and connective tissue within the treatment field. This radiation-induced vascular injury persists for years after treatment and can cause non-healing wounds, tissue necrosis, and bone damage months or even decades later.
Hyperbaric oxygen therapy is the best evidence in radiation tissue injury, and it is among the major reasons patients with such wounds ought to seek a center that has that facility.
Infected and Traumatic Wounds
Burns, crush injuries, lacerations, and puncture wounds that do not granulate or become infected may rapidly deteriorate unless treated in a special environment. Closure is prevented by biofilm, necrotic tissue, and insufficient wound bed preparation. Our team uses the same evidence-based protocols applied to chronic wounds to traumatic wounds, which are not healing on their own.
Why Vascular Health and Wound Healing Cannot Be Separated
Blood is the lifeblood of the healing process in the body. The circulatory system takes oxygen, clotting factors, immune cells, growth factors, and the basic building blocks of new tissue to the wound. Once that delivery system is broken, wound healing will be slowed or halted, no matter what is applied to the wound surface.
This is the reason why wound care with an on-site Vascular Laboratory is a significant clinical benefit to Heart and Health Medical. Instead of sending patients to have vascular studies completed and waiting days or weeks to get results, our team can now do arterial and venous duplex ultrasound, ankle-brachial index, and segmental limb pressure measurements in the same location. Once it is determined that vascular disease is a contributing factor, our wound care specialists and vascular team liaise directly to develop a cohesive treatment plan.
In the case of patients with venous insufficiency, such a plan can involve either compression therapy or referral to minimally invasive vein treatment. In the case of patients with arterial disease, wound treatment may require revascularization before treatment. No dressing, no growth factor, and no oxygen chamber can replace proper blood circulation to the wound site. Early detection and response to that factor is what distinguishes centers that heal and those that merely watch wounds.
Treatment Methods We Use
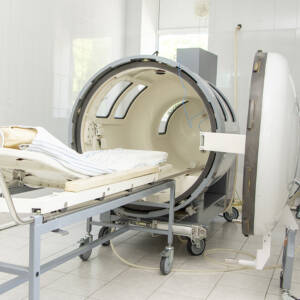
Hyperbaric Oxygen Therapy
Hyperbaric oxygen therapy involves placing the patient in a highly pressurized room with 100 percent pure oxygen at 2 to 3 times the normal atmospheric pressure. In such circumstances, oxygen gets directly dissolved in plasma and gets to the tissues that cannot be supplied adequately by red blood cells alone. The outcomes are high: new blood vessels are stimulated to form, anaerobic bacteria are killed more effectively, the activity of white blood cells is accelerated, and stem cell release is stimulated. HBOT is approved by the FDA for diabetic foot ulcers that are not responding to conventional treatment, radiation tissue injuries, intractable chronic refractory osteomyelitis, and various other wound-related signs.
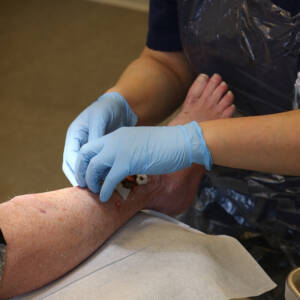
Debridement
Devitalized and necrotic tissue provides an active and hostile environment to healing. It sustains bacterial growth, inhibits migration of new cells over the wound bed, and inhibits the clinician in their judgment of wound depth. Debridement is the removal of tissue by sharp surgical methods, enzymatic agents, or low-frequency ultrasound, based on the nature of the wound and tolerance of the patient. It is usually the most serious action to restart a stalemated wound.
Negative Pressure Wound Therapy
Negative pressure wound therapy – also known as wound VAC – is a wound therapy that uses controlled sub-atmospheric pressure on an enclosed wound using a specially designed foam dressing attached to a small vacuum pump. The negative pressure eliminates the surplus exudate, decreases tissue edema, pulls the wound margins in, minimizes the amount of bacteria, and stimulates the development of granulation tissue mechanically. It specifically works well with large or deep wounds, incisions that have been dehisced, and wounds with a lot of drainage.

Bioengineered Tissue Substitutes
In cases where the wound bed is well-vascularized and clean but the patient has no tissue to close the gap, bioengineered skin substitutes offer living cellular scaffolds that aid in re-epithelialization. These products are derived either out of human dermal fibroblasts, acellular matrix, or bovine collagen and are used to deliver growth factors and structural proteins to the wound. They are clinically indicated to be used in diabetic foot ulcers and venous leg ulcers when other conventional management has not been successful.
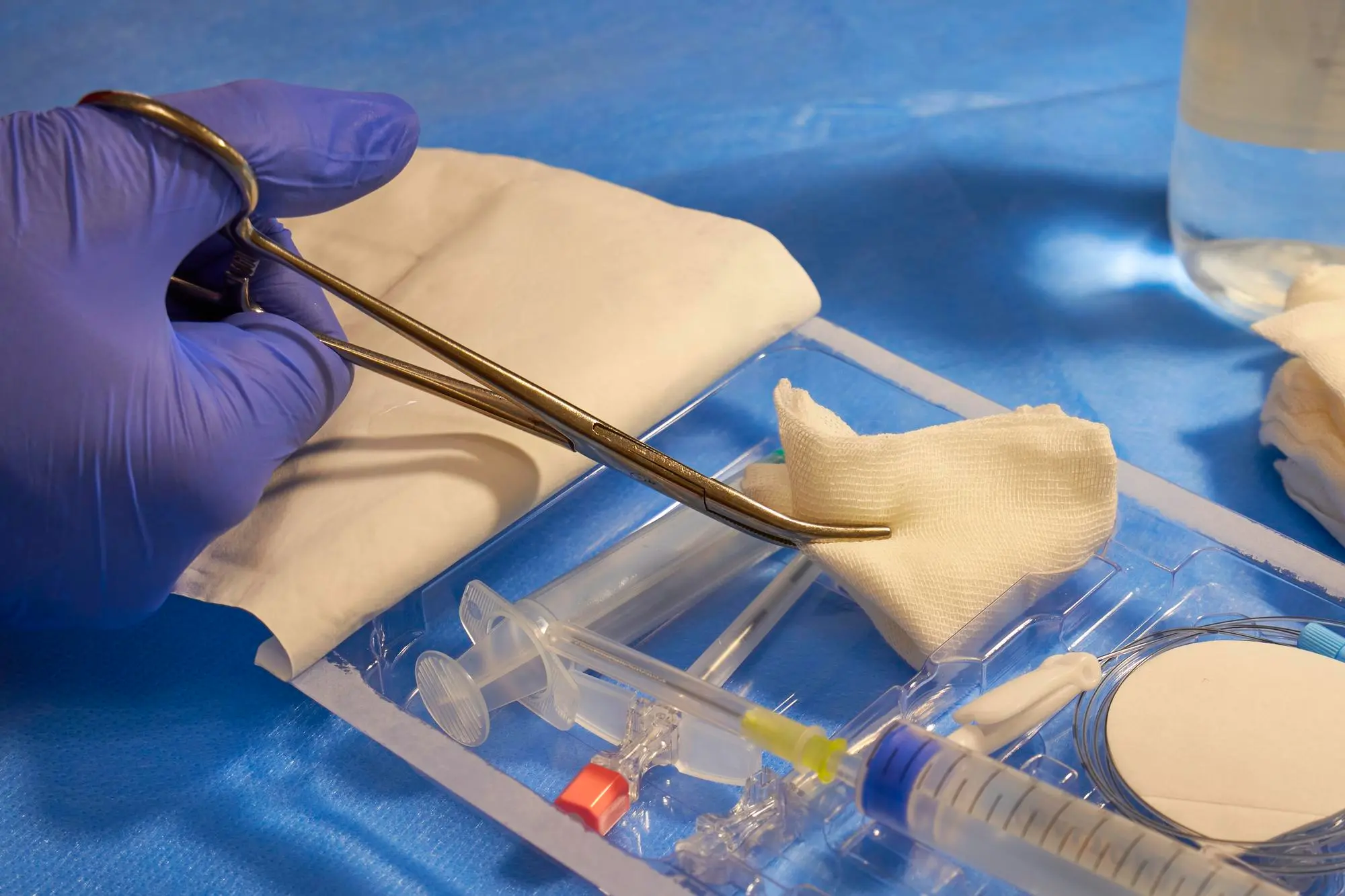
Biologic Dressings
Biologic dressing involves the use of naturally occurring agents – collagen, plant-based biomolecules, and antimicrobial compounds – to promote wound healing as opposed to merely covering the wound. These dressings have anti-inflammatory, antioxidant, and antimicrobial effects. They maintain a humid wound environment that favors cellular activity and minimizes bioburden, which slows down healing. It is selected depending on the current stage of the wound and the clinical presentation.
Low-Frequency Ultrasound
Therapeutic ultrasound is applied to the wound surface to debride, disturb bacterial biofilm, and activate growth factors without making contact with the tissue. The mechanical vibration disrupts slough, bacteria at the cellular level, and triggers resident wound cells to hasten the transition between the inflammatory and the proliferative healing phase. It has a high level of tolerance and can also be useful especially where surgical debridement is not suitable.

Growth Factors and Advanced Topicals
Topical growth factor preparations, including PDGF-based agents with FDA approval for neuropathic diabetic ulcers, are applied directly to the wound to drive cell migration and proliferation. Antimicrobial topicals including silver dressings, cadexomer iodine, and medical-grade honey are used selectively to control infection without damaging viable tissue. Selection is guided by wound culture results and clinical assessment, not routine application.

Total Contact Casting
The clinical standard of offloading diabetic plantar foot ulcers is total contact casting. The cast is made to fit the shape of the foot of the patient and re-distribute the load of the body on the whole plantar surface, removing focal pressure on the wound. Since the patient cannot remove the cast, compliance is ensured – which is a major determinant in outcomes, as when patients are at home, removable offloading devices are often not used.
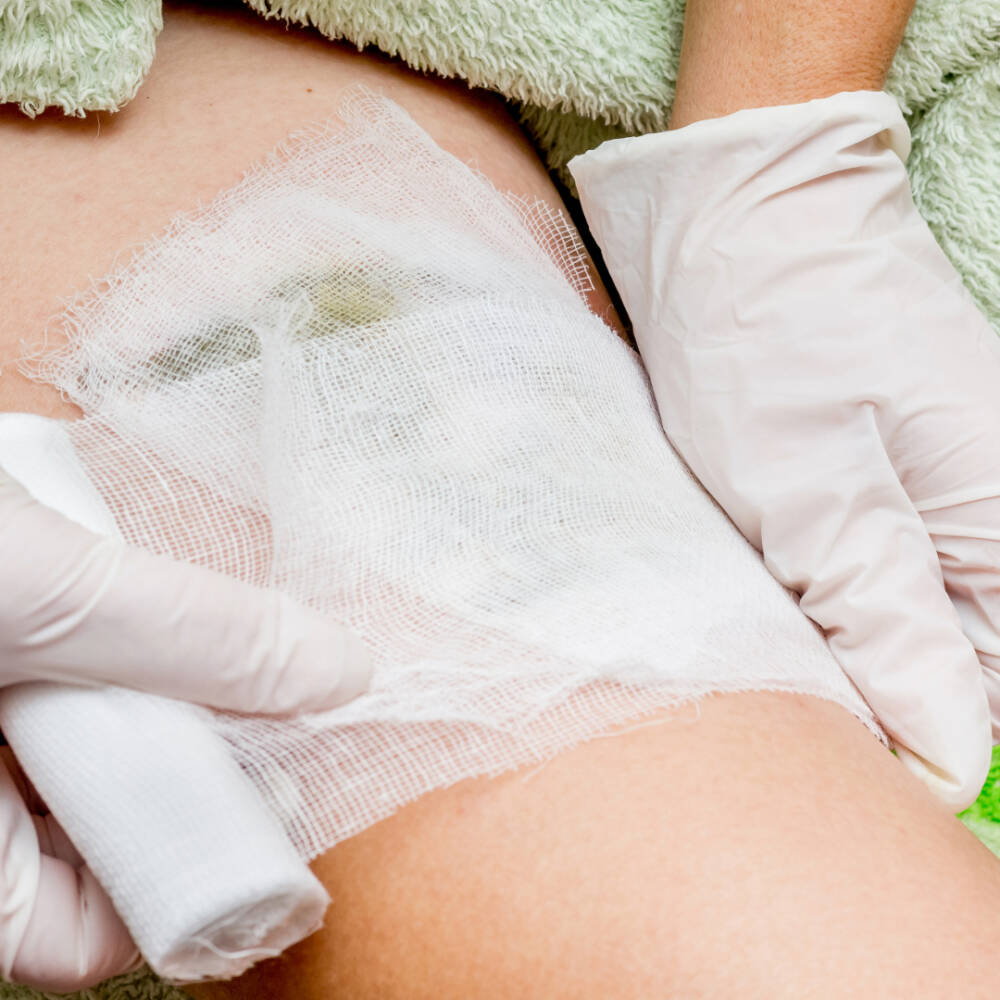
Signs That Require a Wound Care Consultation
Do not apply a bandage and wait if any of the following apply to your wound:
- No measurable improvement after 14 days of home care or primary care treatment
- Increasing pain, redness or swelling around the wound edges
- Discharge that is cloudy, yellow, green or foul-smelling
- Black, gray or leathery tissue in the wound center
- Red streaking extending from the wound toward the body
- Fever or chills accompanying a wound
- Any open wound on the foot or lower leg in a patient with diabetes or known circulation problems
- A wound that has partially closed and then reopened

Steve O. Odeh, M.D.
Steve O. Odeh, M.D. has been in practice for over 20 years and received his certification by the American Board of Surgery in 1998 and Thoracic Surgery in 2000. He received his medical degree from the University of Jos Faculty of Medicine in Nigeria. He completed a research fellowship at the Albert Einstein College of Medicine in New York, followed by a surgical residency at New York Medical College. He completed a cardiothoracic surgery fellowship at SUNY Health Science Center in Brooklyn. He served as Dean of Clinical Services at the University of Sint Eustatius School of Medicine in St. Maarten, and also as Clinical Chair of Surgery at the American University of Antigua College of Medicine in New York, NY. He is a compassionate physician with excellent bedside manners.
Our Provider
Esther Hansen, D.P.M.
Dr. Hansen received her Doctor of Podiatric Medicine at the New York College of Podiatric Medicine and her podiatric surgical residency at the Department of Veterans Affairs Medical Center, Northport, New York. As part of her residency, she was placed with the Leg and Foot Ulcer Group at Stony Brook University Hospital, where she gained specialized clinical knowledge on lower extremity wound care. Before joining Heart and Health, she maintained a private practice for eight years and holds attending and consulting positions at North Shore LIJ Southside and The Hamptons Center for Rehabilitation and Nursing. She is a member of the American Podiatric Medical Association.

Wound Care Articles
The Impact of Poor Circulation on Wound Healing
The Impact of Poor Circulation on Wound Healing Introduction Proper...
Read MoreWhat Are Chronic Wounds and How Are They Treated?
What Are Chronic Wounds and How Are They Treated? A...
Read MoreAntibiotic Stewardship in Wound Care: Managing Resistant Infections – Outline
Antibiotic Stewardship in Wound Care: Managing Resistant Infections – Outline...
Read MoreThe Role of Blood Circulation in Wound Healing
The Role of Blood Circulation in Wound Healing Wound healing...
Read MoreSigns of an Infected Wound
Signs of an Infected Wound Wound infections can turn a...
Read MoreThe Stages of Wound Healing Explained
The Stages of Wound Healing Explained Wound healing is a...
Read MoreAcute vs. Chronic Wounds
Acute vs. Chronic Wounds: Understanding the Difference Wounds are an...
Read MoreSchedule a Consultation
Heart and Health Medical’s Wound Care Center sees patients at our Massapequa location and coordinates care across all Long Island offices.
Call our Massapequa office at 516-804-2100 or request a consultation online. We will schedule you as quickly as possible.
Massapequa
6175 Sunrise Highway, Massapequa, NY 11758
516-804-2100
North Babylon
1350 Deer Park Avenue, North Babylon, NY 11703
631-482-1355
Levittown
1 Center Lane, Levittown, NY 11756
516-550-7223
Coram
3650 Route 112, Coram, NY 11727
631-345-6670
Plainview
1070 Old Country Road, Plainview, NY 11803
516-364-8600

Frequently Asked Questions About Wound Care
The first visit is a full clinical evaluation. We:
- Review your medical history
- Examine and measure the wound
- Assess circulation in the affected area
- Order relevant laboratory work
- Identify contributing conditions
- Develop an individualized treatment plan
You will leave with a clear picture of what is driving your wound and what the treatment path forward looks like.
No. We work alongside your primary care physician, endocrinologist, cardiologist, or any other specialist managing your care. We communicate our findings and treatment plans directly with your providers so your overall care remains coordinated.
Medically necessary wound care services are covered by most of the major health plans such as Medicare. Particular treatments like hyperbaric oxygen therapy are covered based on plan and wound type. We will assist you in explaining your coverage before your first appointment, so call our office.
Active wound care patients are observed weekly or once every two weeks. Intervals can be decreased as the wound advances and the healing becomes regular. During your first appointment, your schedule will be discussed, and will be modified as your wound responds.
Come in. The most consistently harmful decision patients make with non-healing wounds is waiting too long. Wounds that are caught and treated early – before infection spreads to deep tissue or bone – have significantly better outcomes and shorter treatment courses. If your wound has not started healing, make the call today.