Diabetes Treatment
Diabetes is a condition in which there is an increased amount of sugar in the blood. The main factor that plays a role in diabetes is insulin. Insulin is a hormone that is secreted by the pancreas, insulin attaches to cells and allows them to absorb sugar from the bloodstream. Insulin also helps store excess blood sugar in the liver and release it as needed. Without insulin, in the correct amounts, the body cannot regulate blood sugar. There are two distinct types of diabetes; in Type 1, the body is unable to produce insulin. This type is more common in young children and teens. In Type 2, the body does produce insulin, but it is at lower levels, or the body may completely reject the insulin. In non-diabetic patients, food becomes digested, and glucose gets released into the blood. Insulin then transfers the glucose to areas such as liver cells, muscle, and/or fat, where it is stored as a source until it is needed for energy. Patients with diabetes cannot remove glucose from the blood, which results in increased blood sugar levels. Over 30 million or 9.4% of Americans have diabetes, with 23% of those affected undiagnosed and untreated. Eighty-one million or 33.8% of the U.S population have prediabetes and are at high risk for developing Type-2 diabetes.
Type 1 Diabetes
Type 1 diabetes, the body does not make insulin. The immune system attacks and destroys the cells in the pancreas that make insulin. Type 1 diabetes is usually diagnosed in children and young adults, although it can appear at any age. People with type 1 diabetes need to take insulin every day to stay alive.
Type 2 Diabetes
Type 2 diabetes, the body does not make or use insulin effectively. Type 2 diabetes can develop at any age, even during childhood. However, this type of diabetes occurs most often in middle-aged and older people. Type 2 is the most common type of diabetes and is associated with obesity, poor nutrition, and lack of exercise.
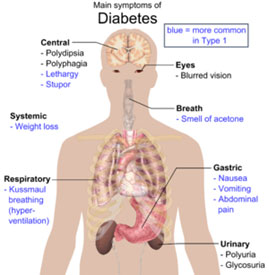
Symptoms of Diabetes Type 1 & Type 2
- Increased thirst
- Frequent urination
- Extreme hunger
- Unexplained weight loss
- Presence of ketones in the urine
- Fatigue
- Irritability
- Blurred vision
- Slow-healing sores
- Frequent infections
Risk Factors For Type 2 Diabetes
- Family History of Diabetes
- Overweight or obese
- Low Levels of Physical Activity and Exercise
- Poor Diet & Nutrition
- High Blood Pressure
- High Cholesterol LDL
- Suffer From Depression
Recommended Lifestyle Change
- Daily Exercise
- Balanced Diet
- Maintain Healthy Body Weight
- Adequate Hydration
- Regular Sleep Cycle
Complications of Diabetes
Over time, high blood glucose leads to problems such as
- heart disease
- stroke
- kidney disease
- eye problems
- dental disease
- nerve damage
- foot problems
Diabetes Treatment:
In general, all people who are diagnosed with diabetes should take control by maintaining a proper diet and exercise plan. They should also be aware of their glucose levels with regular measurements and make sure they take their oral medications and take insulin injections in order to keep their sugar levels at an appropriate level.
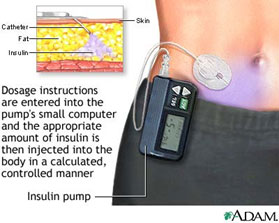
Individuals with Type I diabetes lack the hormone insulin and therefore are required to take insulin. A majority of diabetics receive multiple insulin injections daily or utilize an insulin pump. An insulin pump is an apparatus that is worn outside of the body and it pumps insulin through a bendable tube to a tiny needle that is then inserted beneath the skin. The pump can be programmed to provide small amounts of short-acting insulin continuously throughout the day as well as supplementary doses before meals.
Common Types of Insulin
Rapid-acting insulin: Effective within 15 minutes of injection, at approximately 1 hour it will hit its peak efficiency but continues to work for two to four hours. This is normally taken before a meal and in addition to a long-acting insulin.
Short-acting insulin: Effective within 30 minutes after injection, at approximately 2 to 3 hours it will hit its peak efficiency but continue to work for three to six hours. It is usually given before a meal and in addition to a long-acting insulin regimen.
Intermediate-acting insulin: Effective within 2 to 4 hours after injection, at approximately 4 to 12 hours later it will hit its peak efficiency and continues to work for 12-18 hours. It is usually taken twice a day and in addition to a rapid- or short-acting insulin.
Long-acting insulin: Effective several hours after injection and continues to work for approximately 24 hours. If necessary, it is often used in combination with rapid- or short-acting insulin.
Some Tips on Taking Insulin for Type 1 Diabetes:
- Be sure to acquire your insulin as directed. You should try to take it even if you don’t feel well or are sick.
- Be in contact with your doctor and dietitian and discuss the time you eat and the amount of food you eat, this way your insulin regimen is adjusted suitably to your needs.
- Be consistent with your meals. Try to never skip any meals because your blood sugar can drop to a very low level especially if you have already taken an insulin injection.
- Keep track of your glucose levels on a regular basis as recommended by your doctor.
- Be sure to use your own needles since sharing them can put you at risk for other diseases such as hepatitis C and HIV.
- Store extra insulin in your refrigerator and keep it out of bright light and very hot places.
Individuals with Type 2 diabetes can be in control of their diabetes with regular diet, exercise, and anti-diabetic agents. To be in control of their diabetes some people might require insulin injections a few times a day.
Some Tips on taking oral agents or insulin for diabetes:
- Be familiar on how often to take your medication and be consistent with your schedule.
- Be aware that if the medications aren’t effective, you may have to start using insulin if your blood sugar isn’t lowered.
- Keep in mind that medication alone does not lower blood sugar and that diet and regular exercise play a crucial role.
- If you are overweight, try to lose some weight. Even a small quantity of weight loss can aid in lowering your blood sugar. There is the potential of stopping medication if you can lose the excess weight.
