Cholesterol
To understand high blood cholesterol (ko-LES-ter-ol), it is important to know more about cholesterol.
- Cholesterol is a waxy, fat-like substance that is found in all cells of the body. Your body needs some cholesterol to work the right way. Your body makes all the cholesterol it needs.
- Cholesterol is also found in some of the foods you eat.
- Your body uses cholesterol to make hormones, vitamin D, and substances that help you digest foods.
Blood is watery, and cholesterol is fatty. Just like oil and water, the two do not mix. To travel in the bloodstream, cholesterol is carried in small packages called lipoproteins (lip-o-PRO-teens). The small packages are made of fat (lipid) on the inside and proteins on the outside. Two kinds of lipoproteins carry cholesterol throughout your body. It is important to have healthy levels of both:
- Low-density lipoprotein (LDL) cholesterol is sometimes called bad cholesterol.
- High LDL cholesterol leads to a buildup of cholesterol in arteries. The higher the LDL level in your blood, the greater chance you have of getting heart disease.
- High-density lipoprotein (HDL) cholesterol is sometimes called good cholesterol.
- HDL carries cholesterol from other parts of your body back to your liver. The liver removes the cholesterol from your body. The higher your HDL cholesterol level, the lower your chance of getting heart disease.
What Is High Blood Cholesterol?
Too much cholesterol in the blood, or high blood cholesterol, can be serious. People with high blood cholesterol have a greater chance of getting heart disease. High blood cholesterol on its own does not cause symptoms, so many people are unaware that their cholesterol level is too high.
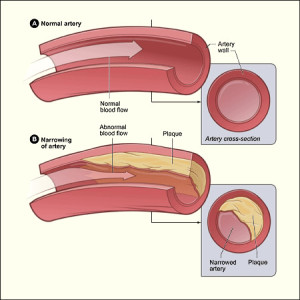
Cholesterol can build up in the walls of your arteries (blood vessels that carry blood from the heart to other parts of the body). This buildup of cholesterol is called plaque (plak). Over time, plaque can cause narrowing of the arteries. This is called atherosclerosis (ath-er-o-skler-O-sis), or hardening of the arteries.
Special arteries, called coronary arteries, bring blood to the heart. Narrowing of your coronary arteries due to plaque can stop or slow down the flow of blood to your heart. When the arteries narrow, the amount of oxygen-rich blood is decreased. This is called coronary heart disease (CHD). Large plaque areas can lead to chest pain called angina (an-JI-nuh or AN-juh-nuh). Angina happens when the heart does not receive enough oxygen-rich blood. Angina is a common symptom of CHD.
Some plaques have a thin covering and can burst (rupture), releasing cholesterol and fat into the bloodstream. The release of cholesterol and fat may cause your blood to clot. A clot can block the flow of blood. This blockage can cause angina or a heart attack.
Lowering your cholesterol level decreases your chance for having a plaque burst and cause a heart attack. Lowering cholesterol may also slow down, reduce, or even stop plaque from building up.
Plaque and resulting health problems can also occur in arteries elsewhere in the body.
Signs and Symptoms of High Cholesterol
There are usually no signs or symptoms of high blood cholesterol. Many people don’t know that their cholesterol level is too high.
Everyone age 20 and older should have their cholesterol levels checked at least once every 5 years. You and your doctor can discuss how often you should be tested.
Diagnosis
High blood cholesterol is diagnosed by checking levels of cholesterol in your blood. It is best to have a blood test called a lipoprotein profile to measure your cholesterol levels. You will need to not eat or drink anything (fast) for 9 to 12 hours before taking the test.
The lipoprotein profile will give information about your:
Total Cholesterol
- Low-density lipoprotein (LDL) bad cholesterol: the main source of cholesterol buildup and blockage in the arteries
- High-density lipoprotein (HDL) good cholesterol: the good cholesterol that helps keep cholesterol from building up in arteries
- Triglycerides: another form of fat in your blood
If it is not possible to get a lipoprotein profile done, knowing your total cholesterol and HDL cholesterol can give you a general idea about your cholesterol levels. Testing for total and HDL cholesterol does not require fasting. If your total cholesterol is 200 mg/dL or more, or if your HDL is less than 40 mg/dL, you will need to have a lipoprotein profile done.
Cholesterol levels are measured in milligrams (mg) of cholesterol per deciliter (dL) of blood. See how your cholesterol numbers compare to the tables below.
LDL Cholesterol Level | LDL-Cholesterol Category |
| Less than 100 mg/dL | Optimal |
| 100-129 mg/dL | Near optimal/above optimal |
| 130-159 mg/dL | Borderline high |
| 160-189 mg/dL | High |
| 190 mg/dL and above | Very high |
HDL Cholesterol Level | HDL Cholesterol Category |
| Less than 40 mg/dL | A major risk factor for heart disease |
| 40–59 mg/dL | The higher, the better |
| 60 mg/dL and above | Considered protective against heart disease |
Triglycerides
Triglycerides can also raise your risk for heart disease. If you have levels that are borderline high (150–199 mg/dL) or high (200 mg/dL or more), you may need treatment.
- Overweight
- Physical inactivity
- Cigarette smoking
- Excessive alcohol use
- Very high carbohydrate diet
- Certain diseases and drugs
- Genetic disorders
Treatment
The main goal of cholesterol-lowering treatment is to lower your low-density lipoprotein (LDL) level enough to reduce your risk for having a heart attack or diseases caused by hardening of the arteries. In general, the higher your LDL level and the more risk factors you have, the greater your chances of developing heart disease or having a heart attack. (A risk factor is a condition that increases your chance of getting a disease.)
Some people are at high risk for heart attack because they already have heart disease. Other people are at high risk for developing heart disease because they have diabetes or a combination of risk factors for heart disease. Follow the steps below to find out your risk for getting heart disease. Talk with your doctor about lowering your risk.
Check the list to see how many of the risk factors you have. These are the risk factors that affect your LDL goal:
- Cigarette smoking
- High blood pressure (140/90 mg/dL or higher), or if you are on blood pressure medicine
- Low high-density lipoprotein (HDL) cholesterol (less than 40 mg/dL)1
- Family history of early heart disease (heart disease in father or brother before age 55; heart disease in mother or sister before age 65)
- Age (men 45 years or older; women 55 years or older)
If you have two or more of the risk factors in the list above, use the NHLBI 10-Year Risk Calculator to find your risk score. Risk scores refer to the chance of having a heart attack in the next 10 years, given as a percentage. Speak with your doctor who may be able to help you by prescribing medication similar to crestor generic to aid with treating high cholesterol.
Use your medical history, number of risk factors, and risk score to find your risk for developing heart disease or having a heart attack according to the table below.
If You Have | You Are in Category | And Your LDL Goal Is |
| Heart disease, diabetes, or risk score more than 20% | I. High Risk | Less than 100 mg/dL |
| 2 or more risk factors and risk score 10-20% | II. Next Highest Risk | Less than 130 mg/dL |
| 2 or more risk factors and risk score less than 10% | III. Moderate Risk | Less than 130 mg/dL |
| 0 or 1 risk factor | IV. Low-to-Moderate Risk | Less than 160 mg/dL |
Some people in this category are at very high risk because they have just had a heart attack or because they have a combination of heart disease together with diabetes, risk factors that are severe, or metabolic syndrome. If you are at very high risk, your doctor may set your LDL goal even lower, to less than 70 mg/dL. Your doctor may also set the LDL goal at this lower level if you have heart disease alone.
After following the above steps, you should have an idea about your risk for getting heart disease or having a heart attack. There are two main ways to lower your cholesterol in order to lower your risk:
- Therapeutic Lifestyle Changes (TLC)—includes a cholesterol-lowering diet (called the TLC Diet), physical activity, and weight management. TLC is for anyone whose LDL is above goal.
- Drug Treatment—if cholesterol-lowering drugs are needed, they are used together with TLC treatment to help lower your LDL.
Your doctor will set your LDL goal. The higher your risk for heart disease, the lower your LDL goal will be. Using the following guide, you and your doctor can develop a possible plan for treating your high blood cholesterol.
Category I, high risk, your LDL goal is less than 100 mg/dL.
Your LDL Level | Treatment |
| If your LDL is 100 or above | You will need to begin the TLC Diet together with drug treatment. |
| Even if your LDL is below 100 | You should follow the TLC Diet on your own to keep your LDL as low as possible. |
Your LDL goal may be set even lower, to less than 70 mg/dL, if you are at very high risk or if you have heart disease. If you have this lower goal and your LDL is 70 mg/dL or higher, you will need to begin the TLC Diet together with drug treatment.
Category II, moderately high risk, your LDL goal is less than 130 mg/dL.
Your LDL Level | Treatment |
| If your LDL is 130 mg/dL or above | You will need to begin the TLC Diet. |
| If your LDL is 130 mg/dL or more after 3 months on the TLC Diet | You may need drug treatment along with the TLC Diet. |
| If your LDL is less than 130 mg/dL | You will need to follow the Heart Healthy Diet. |
Category III, moderate risk, your LDL goal is less than 130 mg/dL.
Your LDL Level | Treatment |
| If your LDL is 130 mg/dL or above | You will need to begin treatment with the TLC Diet. |
| If your LDL is 160 mg/dL or more after you have tried the TLC Diet for 3 months | You may need drug treatment along with the TLC Diet. |
| If your LDL is less than 130 mg/dL | You will need to follow the Heart Healthy Diet. |
Category IV, low to moderate risk, your LDL goal is less than 160 mg/dL.
Your LDL Level | Treatment |
| If your LDL is 160 mg/dL or above | You will need to begin the TLC Diet. |
| If your LDL is still 160 mg/dL or more after 3 months on the TLC Diet | You may need drug treatment along with the TLC Diet. |
| If your LDL is less than 160 mg/dL | You will need to follow the Heart Healthy Diet. |
Lowering Cholesterol With TLC
TLC is a set of lifestyle changes you can make to help lower your LDL cholesterol. The main parts of TLC are:
- The TLC Diet, which recommends:
- Limiting the amount of saturated fat, trans fat, and cholesterol you eat.
- Eating only enough calories to achieve or maintain a healthy weight.
- Increasing the soluble fiber in your diet. For example, oatmeal, kidney beans, and apples are good sources of soluble fiber.
- Adding cholesterol-lowering foods, such as margarines that contain plant sterol or stanol esters that can help lower cholesterol.
- Weight management:
- Losing weight if you are overweight can help lower LDL. Weight management is especially important for those with a group of risk factors that includes raised triglyceride and/or reduced HDL levels and being overweight with a large waist measurement (40 inches or more for men and 35 inches or more for women). This is called metabolic syndrome and it raises your risk for getting heart disease.
- Physical activity:
- Regular physical activity is recommended for everyone. It can help raise HDL levels and lower LDL levels, and is especially important for those with raised triglyceride and/or reduced HDL levels who are overweight with a large waist measurement. Aim for at least 30 minutes of moderate-intensity activity, such as brisk walking, on most, and referably all, days of the week.
Cholesterol-Lowering Medicines
Along with suggesting that you change the way you eat and exercise regularly, your doctor may prescribe medicines to help lower your cholesterol. Even if you begin drug treatment, you will need to continue TLC. TLC lowers your risk not only by lowering LDL but also in other ways and helps keep down the dose of LDL-lowering medication you have to take. Drug treatment controls but does not “cure” high blood cholesterol. Therefore, you must continue taking your medicine to keep your cholesterol level in the recommended range.
The five major types of cholesterol-lowering medicines are:
- Statins
- Very effective in lowering LDL (bad) cholesterol levels
- Safe for most people
- Rare side effects to watch for are muscle and liver problems
- Bile Acid Sequestrants (seh-KWES-trants)
- Help lower LDL cholesterol levels
- Sometimes prescribed with statins
- Not usually prescribed as the only medicine to lower cholesterol
- Nicotinic (Nick-o-TIN-ick) Acid
- Lowers LDL cholesterol and triglycerides, and raises HDL (good) cholesterol
- Should only be used under a doctor’s supervision
- Fibrates
- Lower triglycerides
- May increase HDL (good) cholesterol levels
- When used with a statin, may increase the chance of muscle problems
- Ezetimibe
- Lowers LDL cholesterol
- Acts within the intestine to block cholesterol absorption
When you are under treatment, you will be checked regularly to:
- Make sure your cholesterol level is controlled
- Check for other health problems
You may take medicines for other health problems. It is important that you take ALL medicines as your doctor prescribes. The combination of medicines may lower your risk for heart disease or heart attack.
When trying to lower your cholesterol or keep it low, it is important to remember to follow your treatments for other conditions you may have, such as high blood pressure. Get help with quitting smoking and losing weight if they are risk factors for you.
