Pulmonary Hypertension
Pulmonary hypertension (PULL-mun-ary HI-per-TEN-shun), or PH, is increased pressure in the pulmonary arteries. These arteries carry blood from your heart to your lungs to pick up oxygen.
PH causes symptoms such as shortness of breath during routine activity (for example, climbing two flights of stairs), tiredness, chest pain, and a racing heartbeat. As the disease worsens, its symptoms may limit all physical activity.
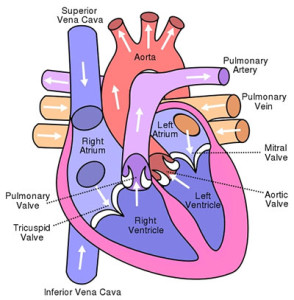
Overview of Pulmonary Hypertension
The lower right chamber of your heart, the right ventricle (VEN-trih-kul), pumps blood to your pulmonary arteries. The blood then travels to your lungs, where it picks up oxygen. This oxygen-rich blood is pumped to the rest of your body.
Three types of changes can affect pulmonary arteries and cause PH:
- The walls of the arteries tighten.
- The walls of the arteries are stiff at birth or become stiff from an overgrowth of cells.
- Blood clots form in the arteries.
These changes make it hard for the heart to push blood through the arteries and into the lungs. Thus, the pressure in the arteries rises. Also, as a result of the heart working harder, the right ventricle becomes strained and weak.
The heart may become so weak that it can’t pump enough blood to the lungs. This causes heart failure. Heart failure is the most common cause of death in people who have PH.
PH is divided into five groups based on its causes. In all groups, the average pressure in the pulmonary artery is higher than 25 mmHg at rest or 30 mmHg during physical activity. The pressure in a normal pulmonary artery is about 15 mmHg at rest. (The mmHg is millimeters of mercury—the units used to measure blood pressure.)
Usually, other diseases or conditions, such as heart and lung diseases or blood clots, cause PH. Some people inherit the condition. In some cases, the cause isn’t known.
Outlook of Pulmonary Hypertension
PH has no cure. However, research for new treatments is ongoing. The earlier PH is treated, the easier it is to control.
Treatments include medicines, procedures, and other therapies. These treatments can relieve PH symptoms and slow the progress of the disease. Lifestyle changes also can help control symptoms.
Signs and Symptoms of Pulmonary Hypertension
Signs and symptoms of pulmonary hypertension (PH) may include:
- Shortness of breath during routine activity, such as climbing two flights of stairs
- Tiredness
- Chest pain
- A racing heartbeat
As PH worsens, you may find it hard to do any physical activities. At this point, other signs and symptoms may include:
- Feeling lightheaded, especially during physical activity
- Fainting at times
- Swelling in your legs and ankles
- A bluish color on your lips and skin
Diagnosing Pulmonary Hypertension
Your doctor will diagnose pulmonary hypertension (PH) based on your medical and family histories, a physical exam, and the results from tests and procedures.
PH can develop slowly. In fact, you may have it for years and not know it. This is because the disease has no early symptoms.
When symptoms do develop, they’re often like those of other heart and lung conditions, such as asthma. This makes PH hard to diagnose.
Medical and Family Histories
To learn about your medical history, your doctor may ask about your signs and symptoms and how and when they began. He or she also may ask whether you have other medical conditions that can cause PH.
Your doctor also may ask whether you have any family members who have or have had PH. People who have a family history of PH are at increased risk for the condition.
Physical Exam
During the physical exam, your doctor will listen to your heart and lungs with a stethoscope. He or she also will check your ankles and legs for swelling and your lips and skin for a bluish tint. These are signs of PH.
Diagnostic Tests and Procedures
You may need tests and procedures to confirm a diagnosis of PH and to look for the underlying cause of the disease. Your doctor also will use test results to find out the severity of your PH.
Tests and Procedures To Confirm a Diagnosis
Echocardiography
This test uses sound waves to create a moving picture of your heart. Echocardiography (EK-o-kar-de-OG-ra-fee) can estimate the pressure in your pulmonary arteries. The test also can show the size and thickness of your right ventricle and how well it’s working.
Chest X-ray
A chest x-ray takes pictures of your heart and lungs. This test can show whether your pulmonary arteries and right ventricle are enlarged. The pulmonary arteries and right ventricle may get larger if the right ventricle has to work hard to pump blood through the pulmonary arteries.
Also, a chest x-ray may show signs of underlying lung disease that may be causing or contributing to PH.
EKG (electrocardiogram)
An EKG is a simple test that shows how fast your heart is beating. It also shows whether your heart’s rhythm is steady or irregular. An EKG may show whether your right ventricle is enlarged or strained.
Right heart catheterization
This procedure measures the pressure in your pulmonary arteries. It also shows how well your heart is pumping blood to the rest of your body. Right heart catheterization (KATH-e-ter-i-ZA-shun) can find any leaks between the left and right sides of the heart.
During this procedure, a thin, flexible tube called a catheter is put into a blood vessel in your groin (upper thigh) or neck. The tube is then threaded into the right side of your heart and into the pulmonary arteries. Through the tube, your doctor can do diagnostic tests and test treatments on your heart.
Tests To Look for the Underlying Cause of Pulmonary Hypertension
Lung function tests
Lung function tests measure the size of your lungs, how much air you can breathe in and out, how fast you can breathe air out, and how well your lungs deliver oxygen to your blood. These tests can help find an underlying lung disease that may be causing PH.
Overnight oximetry
This test measures the level of oxygen in your blood overnight. A low oxygen level during sleep is common in PH, and it can cause the condition to worsen.
For this test, a small light is attached to your fingertip, earlobe, or toe. A machine that’s attached to the light measures the amount of oxygen in your blood throughout the night. In the morning, the light is removed and your oxygen levels are recorded. Overnight oximetry can be done at home or in a sleep lab.
Lung ventilation/perfusion (VQ) scan
This test measures air and blood flow in your lungs. A lung VQ scan can show whether there are blood clots in your lung’s blood vessels.
Blood tests
Blood tests are used to rule out other diseases, such as HIV, liver disease, and autoimmune diseases like rheumatoid arthritis.
Exercise testing
Exercise testing consists of either a 6-minute walk test or a cardiopulmonary exercise test. These tests can help find out whether another disease or condition is causing your symptoms.
A 6-minute walk test measures the distance you can quickly walk in 6 minutes. A cardiopulmonary exercise test measures how well your lungs and heart work while you exercise on a treadmill or bicycle.
Finding Out the Severity of Pulmonary Hypertension
Exercise testing is used to find out how severe PH is. During this test, your doctor will rate your activity level. Your level is linked to how severe your PH is. The rating system ranges from class 1 to class 4.
- Class 1 has no limits. You can do regular physical activities, such as walking or climbing stairs. These activities don’t cause PH symptoms, such as tiredness, shortness of breath, or chest pain.
- Class 2 has slight or mild limits. You’re comfortable while resting, but regular physical activity causes PH symptoms.
- Class 3 has marked or noticeable limits. You’re comfortable while resting. However, walking even one or two blocks or climbing one flight of stairs can cause PH symptoms.
- Class 4 has severe limits. You’re not able to do any physical activity without discomfort. You also may have PH symptoms while at rest.
Over time, you may need more exercise tests to find out how well your treatments are working. Each time testing is done, your doctor will compare your activity level to the previous one.
Treatment for Pulmonary Hypertension
Pulmonary hypertension (PH) has no cure, but treatment may help relieve symptoms and slow the progress of the disease.
PH is treated with medicines, procedures, and other therapies. Treatment will depend on what type of PH you have and how severe it is. (For more information, see “Types of Pulmonary Hypertension.”)
Group 1 Pulmonary Arterial Hypertension
This type of PH includes PH that is inherited, that has no known cause, or that is caused by certain conditions. Treatment for group 1 pulmonary arterial hypertension (PAH) includes medicines or medical procedures.
Medicines
If you have group 1 PAH, you may need medicines to relax the blood vessels in your lungs and reduce excess cell growth in the blood vessels. As the blood vessels relax, more blood can flow through them.
Examples of these medicines include phosphodiesterase-5 inhibitors, prostanoids, endothelin receptor antagonists, and calcium channel blockers.
To find out which of these medicines will work best, you’ll likely have an acute vasoreactivity test. This test shows how the pressure in your pulmonary arteries reacts to certain medicines. This test is done during right heart catheterization.
Medical and Surgical Procedures
If you have group 1 PAH, you may need one or more of the following procedures.
Atrial Septostomy
For this procedure, a thin, flexible tube called a catheter is put into a blood vessel in your leg and threaded to your heart. The tube is then put through the wall that separates your right and left atria (the two upper chambers of your heart). This wall is called the septum.
A tiny balloon on the tip of the tube is inflated to create an opening between the atria. This procedure relieves the pressure in the right atria and increases blood flow. Atrial Septostomy is rarely performed in the United States.
Lung transplant
A lung transplant is a surgery to replace a person’s diseased lung with a healthy lung from a deceased donor. This procedure may be used for people who have a severe lung disease that’s causing PAH.
Heart-lung transplant
A heart-lung transplant is a surgery in which both the heart and lungs are replaced with healthy organs from a deceased donor.
Group 2 Pulmonary Hypertension
Group 2 PH is caused by conditions that affect the left side of the heart, such as mitral valve disease. Treating these conditions also will help treat PH. Treatments may include lifestyle changes, medicines, and surgery.
Group 3 Pulmonary Hypertension
Group 3 PH is linked to lung conditions, such as COPD (chronic obstructive pulmonary disease) and interstitial lung disease. Group 3 PH also may be linked to certain sleep disorders, such as sleep apnea.
If you have this type of PH, you may need oxygen therapy. This treatment raises the level of oxygen in your blood. You’ll likely get the oxygen through soft, plastic prongs that fit into your nose. You can get oxygen therapy at home or in a hospital.
Your doctor also may recommend other treatments if you have an underlying lung disease.
Group 4 Pulmonary Hypertension
This type of PH is due to blood clots in the lungs, blood clotting disorders, or sickle cell anemia. If you have this type of PH, your doctor will likely prescribe anticoagulants, or “blood thinners.” These medicines prevent clots from forming or from getting larger.
In some cases, surgery is used to remove scarring in the pulmonary arteries due to old blood clots.
Group 5 Pulmonary Hypertension
Various diseases and conditions cause group 5 PH. Examples include sarcoidosis, Langerhans cell histiocytosis, and lymphangioleiomyomatosis (LAM). This type of PH also may be due to an object, such as a tumor, pressing on the pulmonary blood vessels.
This type of PH is treated by treating its cause.
All Types of Pulmonary Hypertension
Several treatments may be used for all types of PH. These treatments include:
- Diuretics, or “water pills.” These medicines help reduce fluid buildup in your body, including swelling in your ankles and feet.
- Blood-thinning medicines. These medicines help prevent blood clots from forming or getting larger.
- Digoxin. This medicine helps the heart beat stronger and pump more blood. Digoxin is sometimes used to control the heart rate when certain abnormal heart rhythms occur, such as atrial fibrillation or atrial flutter.
- Oxygen therapy. This treatment raises the level of oxygen in your blood.
- Physical activity. Regular activity may help improve your ability to be active. Your doctor can help you create an exercise plan that’s safe for you.
Research on new treatments for PH is ongoing. These treatments offer hope for the future. Talk to your doctor about whether you should consider participating in research studies.
